Covid-19 Inquiry

Module 3: healthcare
Report and Recommendations
About Covid-19
Covid-19 is a virus.
It suddenly appeared in the UK in 2020. It spread very quickly.
People across the world became ill. Many people died. This meant it was called a pandemic.

The 4 governments of the UK had to make big decisions about how to protect people.

- UK Government
- Welsh Government
- Scottish Government
- Northern Ireland Executive
The Covid-19 Inquiry

The Inquiry is finding out what happened during the pandemic.

This will help people to make better decisions in the future.

The Inquiry has hearings. At a hearing, we listen to people like politicians, doctors and scientists.

After the hearings, the Chair, Baroness Hallett, produces reports.

This Easy Read is about her report for Module 3.
About this report

This is an Easy Read version of the Covid-19 Inquiry’s 3rd report.

The full report has a lot more information.

There are more versions in accessible formats and languages.

You can get all the reports from the Inquiry website:
Healthcare

This report is about how healthcare was affected by the pandemic.

Healthcare means the care and treatment that people got from, for example:

• Hospitals
• Ambulances
• NHS 111

We found out what the pandemic was like for healthcare workers like doctors and nurses and patients.
Things we found out

We were not ready for a pandemic.

Healthcare organisations were already struggling.
The pandemic was devastating.

The Inquiry’s Chair, Baroness Hallett, said: “We coped, but only just.”

We only managed to cope because healthcare staff worked extremely hard.
Getting healthcare
Some people did not get the health care they would normally get.
Some people were not in hospital when they needed to be.

Some people waited in ambulances for hours.
There was not enough staff or hospital equipment.
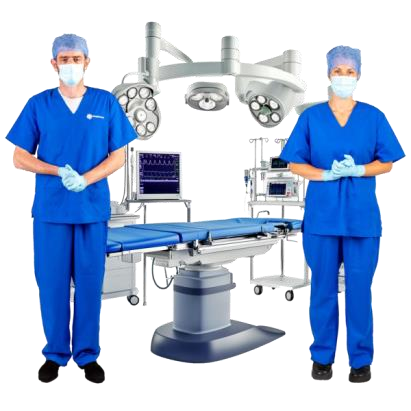
Millions of operations were cancelled, and serious illnesses were not found out or treated.
End of life plans
Sometimes, plans were made in advance to say that doctors should not try to restart someone’s heart if it stopped beating.

Some of these plans should not have been made.
Some families and carers found out about the plans after the person had died.
Healthcare workers

Healthcare staff had to work very hard for many months.

It affected their mental health.
Many healthcare workers died

Many of the workers who died were ethnic minorities.
Ethnic means the culture or background you are from.
Minority means the size of a group of people is smaller than the total number of people in a country.
Planning healthcare

Hospitals need better plans about how to deal with a pandemic.

The plans need to be about making sure there are more beds, more equipment and more staff in a pandemic.
Stopping the virus

At the start of the pandemic, people did not know that the virus could spread through the air.

This meant that advice about how to avoid spreading the virus was not enough to stop it.
People with other illnesses

Some people were more at risk from Covid-19.

They had to stay at home, away from other people, called shielding.
Information about shielding was not good enough.
Rules about visiting people

People were not allowed to visit friends and relatives in hospital.
Many people died alone.

This was extremely upsetting for everyone.
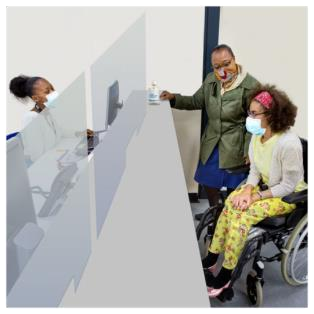
The rules also meant that people did not have the support they needed in medical appointments.

This included pregnant women, people with dementia, and people with learning disabilities.
111 services

People with Covid-19 symptoms were told to phone 111.
Lots of people used the service.

This meant it took a long time to get an answer. Some people gave up before their call was answered.
Long Covid

People who are still ill with Covid for a long time have ‘Long Covid’.
It took a long time for people to find out why they were so unwell.
People in some parts of the UK still do not get good treatment for Long Covid.
What should happen next

These are things governments must do to protect people in the future.

1. Emergency care
Make sure hospitals are ready to quickly treat a big number of people if there is another pandemic.

2. Trying to stop infections
Involve more people in making decisions about how to stop people getting ill.

3. Collect and use information
Collect information about who is most likely to become unwell in a pandemic.
Use the information to keep them safe.

Keep better records about the deaths of healthcare workers.

4. Planning people’s care
Involve people in planning their own care.
People should have a plan that says what they want to happen to them if they are very unwell.

5. Support healthcare workers
Healthcare staff are more likely to cope if they get good support.
They are also more likely to stay in their jobs.

6. Making decisions
Write guidance for decision-makers to follow in emergencies.
For example, if critical care wards can’t deal with the number of patients.
Critical care is for people who are very unwell.
What happens next

After every hearing Baroness Hallett writes her recommendations.

All these recommendations are designed to work well together and they should happen at the same time as the recommendations from the Inquiry’s 1st and 2nd report.

She listened to all the hearings then wrote the recommendations.
She expects that all the recommendations will be done by the UK’s governments.

She will check to make sure this is happening.
Future reports

There will be more reports about:
- vaccines and treatments

- things that were bought – like medical equipment and software
- test, trace and isolate

- social care
- children and young people

- how the governments in the UK spent money
- how it affected the whole population
Find out more

If you want to find out more, please go to this website.

Thank you for reading our report.